ADHD – what you need to know
ADHD – what you need to know
When I was considering my options for re-training and returning to university so that I could work in the mental health field I thought long and hard about which path I wanted to pursue: psychology, social work, counselling/psychotherapy. There were a bunch of things that played into the decision I took, one of which was that I didn’t think that I wanted to work within a medicalised model of mental healthcare that prioritised assessment and diagnosis of mental illness at its core. Fast-forward many years and I find myself reflecting on the number of times I’ve conducted the ASRS screen (one of the tools we use to explore whether someone has a pattern of behaviours that might warrant exploring a thorough ADHD assessment). And I’ve been seriously reflecting how this happened!
To begin with I blamed the fact that so many of my clients had downloaded TikTok during the COVID-19 lockdowns where there was a blooming of ADHD symptom-sharing and honestly I was a bit dismissive (bad therapist)…but then I spent time doing two really important things: firstly, I really listened to what my clients were saying to me about some of the symptoms and experiences they were struggling with. And then I went into full research mode.
What is ADHD?
To succinctly summarise ADHD is quite tricky but here’s the best I can manage at the moment: attention-deficit/hyperactivity disorder (ADHD) is a complex, lifelong neurodevelopmental disorder that includes a combination of persistent problems, such as difficulty paying attention, hyperactivity and impulsive behavior. Adult ADHD can lead to unstable relationships, poor work performance, low self-esteem, and other problems.
What ADHD can look like:
Hyperactive
- Excessive talking
- Speaking very quickly
- Gets off-topic often
- Unintentionally loud
- Rambling tangents
- Fidgeting when being spoken to
Impulsive:
- Interrupting
- Blurting out answers
- Impatient waiting for turn
- Lacking internal filter
- Quick emotional responses
- Inappropriate oversharing
- May unintentionally dominate conversations
Inattentive:
- Zoning out
- Struggling to pay attention*
- Getting bored easily*
- Forgetting details*
- Often needing things to be repeated
- Distracted by background noise / external stimuli
*unless very interested in the topic/conversation
Why the spike in diagnoses?
I was then super curious about why I was suddenly having this conversation over and over again in session – clearly it wasn’t just about TikTok! This one is a complicated because it’s very multifactorial in nature, and I’m just sharing some of my thoughts and observations on this:
- ADHD has historically been diagnosed in children and therefore a whole bunch of now adults missed out on having their symptoms appropriately recognised until maybe their own children have been diagnosed and they started to wonder about their own experience.
- ADHD, like many health conditions has had a historic gender-skew with it more frequently being diagnosed in boys. In recent years, there’s been a greater appreciation that ADHD, like a range of other conditions (don’t get me started), shows up differently in girls, women and people who identify as women.
- The COVID-19 lockdowns saw some significant changes in our environment that had knock-on effects for people who had been living with previously undiagnosed ADHD which saw their usual structures and practices that they’d used to adaptively manage the symptoms no longer be available or work for them.
- The TikTok (social media more broadly) phenomenon has played a part I think – more people sharing their lived experiences in real-life settings and in an accessible way as opposed to the clinical / classroom perspective has caused many more people to exclaim, “wow, that’s what I’m like.”

Trauma and ADHD
The literature is pretty clear. There’s a significant overlap between trauma and ADHD – I strongly recommend that you watch/listen to this interview on Steven Bartlett’s show with Dr Daniel Amen. Dr Amen is a Psychiatrist who uses FMRI brain scans to help in his diagnostic process and he brilliantly articulates the effect of emotional trauma on the brain and how it mirrors / connects to ADHD.
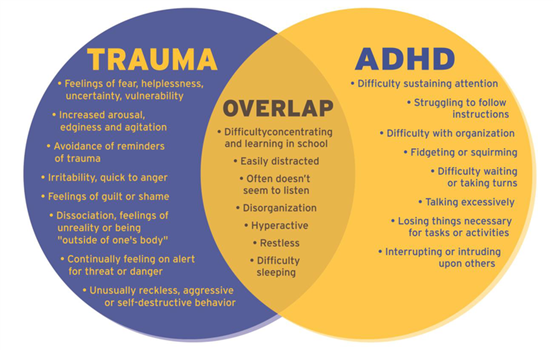
I think our historic misunderstanding of trauma has resulted in a lot of confusion and misdiagnosis – in a number of mental health intersections. I do think that there’s a very nuanced and complicated relationship at play where the nature of the trauma, the age of the person and the support / therapeutic interventions available all play a role. As with trauma, ADHD has to be considered from the perspective of the individual, whilst our systems (mental health model) are focused on generalisation of symptoms, because this aids the process of diagnosis. However, with all our recent developments in neuroscience we are now better able to see that the overlap and interconnection between these two is very real. I might leave a further unpacking of this topic to another blog but for now, here’s an image that I think summarises things:
Resources and suggestions:
Australian resources:
ADHD Australia: https://www.adhdaustralia.org.au/
ADHD Foundation: https://adhdfoundation.org.au/
National Guidelines: https://aadpa.com.au/guideline/
Women and ADHD:
Dr Louise Newson’s podcast interview with ADHD expert Dr David Chapman: “ADHD and hormones” https://open.spotify.com/episode/11lhLSRK4tBCL5Lfq1pAtw?si=55d8f2c8906444da
Em Rusciano’s Press Club speech: https://youtu.be/4v88Wd20GiU
Mia Freedman: https://www.mamamia.com.au/podcasts/no-filter/mia-freedman-adhd/
ABC article: https://www.abc.net.au/news/2022-02-18/adult-women-face-barriers-getting-adhd-diagnosis-treatment/100613218
CHADD: https://chadd.org/for-adults/women-and-girls/
Podcasts / You Tube:
Huberman Lab: https://hubermanlab.com/adhd-and-how-anyone-can-improve-their-focus/
How to ADHD: https://www.youtube.com/c/HowtoADHD/featured
ADHD and Executive Function: https://youtu.be/GR1IZJXc6d8
Gabor Maté on Joe Rogan: https://youtu.be/4jQSOSi2DA8
I have ADHD podcast: https://ihaveadhd.com/podcast/
If you need support around ADHD, we have a team of experienced therapists at Thea Baker Wellbeing – please reach out to us at: hello@theabaker.com.au / 03 9077 8194.
